
Non-urgent medical procedures were deferred at the start of the pandemic, freeing up hospitals to treat Covid-19 patients.ST PHOTO: KUA CHEE SIONG
Updated from : The Straits Times, 25 June 2020
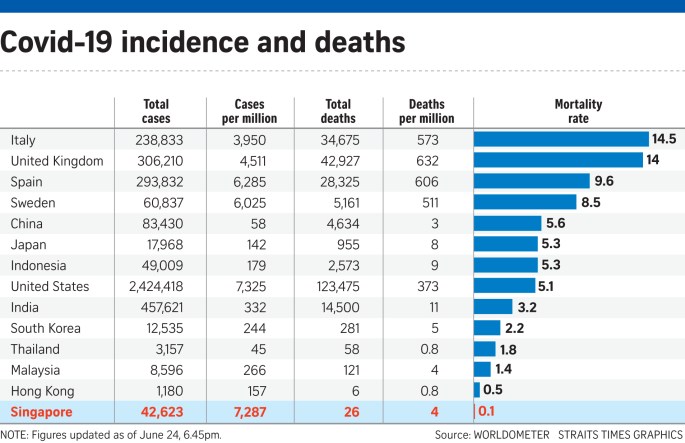
Patients with Covid-19 are faring far better in Singapore than in most places in the world, with 26 deaths out of more than 42,000 infected.
Experts say this is because the vast majority of those infected are young and healthy workers and because the healthcare system here has never been overwhelmed, so patients are all able to receive the best care possible.
Foreign workers living in dormitories account for more than 90 per cent of all cases here. Being younger and healthier, they have generally suffered from a milder illness.
Because the Government started deferring non-urgent medical procedures at the start of the pandemic, hospitals here were freed up to treat Covid-19 patients.
This allowed patients who are sicker to get close monitoring and quick treatment to reduce their risk of getting seriously ill.
Professor Dale Fisher, a senior infectious diseases consultant at the National University Hospital, said the number of deaths has been relatively low because of the younger and healthier cohort and the fact that “we were never overwhelmed in hospitals or ICUs”.
Dr Ling Li Min, a senior consultant at the National Centre for Infectious Diseases (NCID), agreed that the “provision of better initial treatment has contributed to the smaller number of ICU cases”.
Parameters such as heart rate, blood pressure and oxygenation are monitored at least six times daily, and the medical team reviews these patients at least once a day, she said.
The moment a patient takes a turn for the worse and requires oxygen support, he is placed on the intensive care unit (ICU) team’s “watch list” – even though he remains in the normal ward – and the frequency of monitoring increases, she explained.
“Once there is further deterioration, the ICU team will review and transfer the patient to the ICU if needed,” she said.
Early admission of such patients to the ICU is possible when there are not that many extremely ill patients. In the ICU, they are more closely monitored and may even be put on a ventilator to help them breathe before it becomes absolutely necessary.
Some might not actually need it, but it is better for such mechanical aid to be in place than for the patient to need “crash intubation”, explained Associate Professor Hsu Liyang, an infectious diseases doctor and epidemiologist at the National University of Singapore’s Saw Swee Hock School of Public Health.
Crash intubation refers to a life-saving emergency insertion of a breathing tube, when the patient is fighting for breath.
Dr Ling credited clinicians at the NCID, which has about 130 of the 200 hospitalised Covid-19 patients, for being “astute with identifying patients who will deteriorate” and for ensuring seamless and quick transfer of care to ICU teams.
And the ICU teams “are spot-on in identifying patients who will need intubation early versus those who do not require it”, she said.
These interventions have helped keep the death rate low.
Since April, patients with pneumonia and who need oxygen have been placed in a prone position for five one-hour sessions a day, resulting in the vast majority not needing ventilator care.
Eligible patients are given the option to participate in clinical trials for treatment. This may give them better outcomes.
Dr Ling added that community-based testing has also picked up asymptomatic individuals, which means the actual number of symptomatic patients is much lower than the headline numbers.
Such testing also means that those who need it are sent to hospital early, resulting in better care.

You must be logged in to post a comment.